التهاب الردب
| التهاب الردب | |
|---|---|
 | |
| الأمعاء الغليظة (sigmoid colon) تـُبدي عدة رتوج. الرتوج البادية على جانبي حزمة العضلات الطولية (taenium). | |
| التبويب والمصادر الخارجية | |
| التخصص | طب الجهاز الهضمي, جراحة عامة[*] |
| ICD-10 | K57. |
| ICD-9-CM | 562 |
| DiseasesDB | 3876 |
| MedlinePlus | 000257 |
| eMedicine | med/578 |
| Patient UK | فشل عرض الخاصية P1461: لم يتم العثور على الخاصية P1461. التهاب الردب |
| MeSH | D004238 |
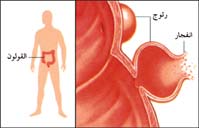
التهاب الردب/الرتج إنگليزية: Diverticulitis مرض شائع من أمراض القولون (الأمعاء الغليظة). ومن أعراضه ألم في الجانب الأيسر أسفل البطن مصحوب بحمى. ويتطور المرض من مرض الرُّتاج، وهو اضطراب واسع الانتشار بين متوسطي الأعمار والمسنين في البلاد المتقدمة.
ويتميز التهاب الرتج بوجود انتفاخات على الجدار الخارجي للقولون تُسمى الرتوج. ونادرًا ما يصيب التهاب الرتج الأشخاص الذين تقل أعمارهم عن الثلاثين عامًا. ولا تظهر أية أعراض على معظم المصابين بالتهاب الرتج. وقد ظل الأطباء لسنوات عديدة يعتقدون أن الوجبة الغذائية المحتوية على نسب قليلة من الخشائن (ألياف الفواكه والخضراوات) قد تساعد في منع التهاب الرتج، غير أن الشواهد في هذه الأيام قد أثبتت العكس إذ إن نقص الخشائن في الوجبة الغذائية يجعل الفضلات في القولون أكثر التصاقًا وأكثر لزوجة ولا تتحرك في القولون بسهولة. ويسبب ذلك ضغطًا ينتج عنه انتفاخ الغشاء الداخلي للقولون في العديد من النقاط الضعيفة، مما يؤدي إلى تكوين انتفاخات صغيرة دائمة، يمكن أن تُرى عن طريق الفحص بالأشعة السينية. ونادرًا ما تحدث هذه الحالة بين سكان البلاد النامية، ذلك لأن نسبة الألياف عالية في الوجبة الغذائية العادية عندهم.
ويتطور التهاب الرتج في حالات كثيرة من الرتاج. ويحدث هذا عندما يلتهب أحد الرتوج أو عدد منها. وقد تنفجر الانتفاخات الملتهبة وتلوث المادة التي تخرج منها السطح الخارجي للقولون. وتنحصر الإصابة في معظم الحالات في منطقة صغيرة، غير أنها تنتشر وتتطور إلى التهاب الصِّفاق، وهو مرض خطير قد يسبب الوفاة.
الأسباب
تتكون الرتوج عادة في القولون السيني وذلك لكون الضغط الداخلي هو الأعلى فيه من بين أجزاء القولون الأخرى. كما أن نقص الغذاء بالألياف. يعتقد أن التهاب الرتوج ينتج عن انسداد أحد الرتوج - بقطعة من البراز أو طعام ربما - مما يؤدي التهابها.
المضاعفات
- انسداد معوي
- خراج
- ناسور
- التهاب الصفاق
- تضيق القولون
ويعالج الأطباء التهاب الرتج بالمضادات الحيوية، للتحكم في الإصابة والسيطرة عليها. ويعالجونه أيضًا بالعقاقير لإحداث ارتخاء في الجدار العضلي للقولون، وبالمركبات الكيميائية للمساعدة في عملية تفريغ القولون. وقد تساعد الوجبة الغذائية المحتوية على نسبة عالية من الألياف، في منع عودة هذا المرض.
التشخيص
People with the above symptoms are commonly studied with computed tomography, or a CT scan.[1] Ultrasound can provide preliminary investigation for diverticulitis. Amongst the findings that can be seen on ultrasound is a non-compressing outpouching of bowel wall, hypoechoic and thickened wall, or an obstructive fecalith at the bowel wall. Besides, bowel wall oedema with adjacent hyperechoic mesentery can also be seen on ultrasound. However, a CT scan is the mainstay of diagnosing diverticulitis and its complications.[2] The diagnosis of acute diverticulitis is made confidently when the involved segment contains diverticula.[3] CT images reveal localized colon wall thickening, with inflammation extending into the fat surrounding the colon.[4] Amongst the complications that can be seen on CT scan are: abscesses, perforation, pylephlebitis, intestinal obstruction, bleeding, and fistula.[2]
Barium enema and colonoscopy are contraindicated in the acute phase of diverticulitis because of the risk of perforation.[5][6]
التصنيف حسب الشدة
Uncomplicated vs complicated
Uncomplicated acute diverticulitis is defined as localized diverticular inflammation without any abscess or perforation.[7] Complicated diverticulitis additionally includes the presence of abscess, peritonitis, obstruction, stricture and/or fistula. 12% of patients with diverticulitis present with complicated disease.[8]
أنظمة التصنيف
At least four classifications by severity have been published in the literature. As of 2015, the 'German Classification'[9] was widely accepted and is as follows:[10]
- Stage 0 – asymptomatic diverticulosis
- Stage 1a – uncomplicated diverticulitis
- Stage 1b – diverticulitis with phlegmonous peridiverticulitis
- Stage 2a – diverticulitis with concealed perforation, and abscess with a diameter of one centimeter or less
- Stage 2b – diverticulitis with abscess greater than one centimeter
- Stage 3a – diverticulitis with symptoms but without complications
- Stage 3b – relapsing diverticulitis without complications
- Stage 3c – relapsing diverticulitis with complications
As of 2022, other classification systems are also used.[9]
The severity of diverticulitis can be radiographically graded by the Hinchey Classification.[11]
Smoldering diverticulitis
In "smoldering diverticulitis" (SmD), there are frequent relapsing symptoms[12] but no progression to diverticular complications.[13] Approximately 5% of people with diverticulitis experience a variant known as smoldering diverticulitis.[14] Smoldering diverticulitis cases make up 4–10% of diverticulitis surgeries.[15]
التشخيصات التفاضلية
The differential diagnoses include colon cancer, inflammatory bowel disease, ischemic colitis, and irritable bowel syndrome, as well as several urological and gynecological processes. In those with uncomplicated diverticulitis, cancer is present in less than 1% of people.[16]
Prognosis
- Estimates for the proportion of people with diverticulosis who will develop diverticulitis range from 5%[17] to 10% to 25%.[18]
- Most people with uncomplicated diverticulitis recover following medical treatment. The median time to recovery is 14 days. Approximately 5% of people experience smoldering diverticulitis.[17]
- Diverticulitis recurs in around one-third of people – about 50% of recurrences occur within one year, and 90% within 5 years. Recurrence is more common in younger people, those with an abscess at diagnosis, and after an episode of complicated diverticulitis.[17]
- About 5% of people with diverticular disease have complications when followed up for 10–30 years. The risk of complications, such as peritonitis or perforation, is greater during the first episode of diverticulitis, and the risk reduces with each recurrence. People who are immunocompromised have a 5-fold increased risk of recurrence with complications, such as bowel perforation, compared to immunocompetent people.[17]
- The decision criteria for having surgical treatment has been subject to debate and development.[19][18][20][21]
- Following surgical treatment, approximately 25% of people remain symptomatic.[17]
Treatment
In uncomplicated diverticulitis, administration of fluids may be sufficient treatment if no other risk factors are present.[22][23]
Diet
Diverticulitis patients may be placed on a low-fiber diet,[24] or a liquid diet,[25] although evidence for improved outcomes through diet has not been found.[23]
Medication
Antibiotics
Mild uncomplicated diverticulitis without systemic inflammation should not be treated with antibiotics.[26][27] For mild, uncomplicated, and non-purulent cases of acute diverticulitis, symptomatic treatment, IV fluids, and bowel rest have no worse outcome than surgical intervention in the short and medium term, and appear to have the same outcomes at 24 months. With abscess confirmed by CT scan, some evidence and clinical guidelines tentatively support the use of oral or IV antibiotics for smaller abscesses (<5 cm) without systemic inflammation, but percutaneous or laparoscopic drainage may be necessary for larger abscesses (>5 cm).[26][28]
Rifaximin was found in a meta-analysis to give symptom relief and reduce complications[29] but the scientific quality of the underlying studies has been questioned.[22]
Mesalamine
Mesalamine is an anti-inflammatory medication used in the treatment of inflammatory bowel diseases.[30] In limited studies, patients with diverticulitis and symptomatic diverticular disease treated with mesalamine have shown improvement in both conditions.[31] Mesalazine may reduce recurrences in symptomatic uncomplicated diverticular disease.[32] In 2022 Germany introduced guidance to use mesalamine to treat acute uncomplicated diverticulitis.[33]
Surgery
Indications for surgery are abscess or fistula formation; and intestinal rupture with peritonitis.[34] These, however, rarely occur.[34]
Emergency surgery is required for peritonitis with perforated diverticulitis[26][28] or intestinal rupture.[35]
Surgery for an abscess or fistula is indicated either urgently or electively. The timing of the elective surgery is determined by evaluating factors such as the stage of the disease, the age of the person, their general medical condition, the severity and frequency of the attacks, and whether symptoms persist after the first acute episode. In most cases, elective surgery is indicated when the risks of the surgery are less than the risks of the complications of diverticulitis. Elective surgery is not indicated until at least six weeks after recovery from the acute event.[36]
Technique
The first surgical approach consists of resection and primary anastomosis. This first stage of surgery is performed on people if they have a well-vascularized, nonedematous, and tension-free bowel. The proximal margin should be an area of the pliable colon without hypertrophy or inflammation. The distal margin should extend to the upper third of the rectum where the taenia coalesces. Not all of the diverticula-bearing colon must be removed, since diverticula proximal to the descending or sigmoid colon are unlikely to result in further symptoms.[37]
Approach
Diverticulitis surgery consists of a bowel resection with or without colostomy. Either may be done by the traditional laparotomy or by laparoscopic surgery.[38] The traditional bowel resection is made using an open surgical approach, called colectomy. During a colectomy, the person is placed under general anesthesia. A surgeon performing a colectomy will make a lower midline incision in the abdomen or a lateral lower transverse incision. The diseased section of the large intestine is removed, and then the two healthy ends are sewn or stapled back together. A colostomy may be performed when the bowel has to be relieved of its normal digestive work as it heals. A colostomy implies creating a temporary opening of the colon on the skin surface, and the end of the colon is passed through the abdominal wall with a removable bag attached to it. The waste is collected in the bag.[39]
However, most surgeons prefer performing the bowel resection laparoscopically, mainly because postoperative pain is reduced with faster recovery. Laparoscopic surgery is a minimally invasive procedure in which three to four smaller incisions are made in the abdomen or navel. After incisions into the abdomen are made, placement of trocars occurs, which allows a camera and other equipment to enter the peritoneal cavity. The greater omentum is reflected, and the affected section of the bowel is mobilized. Alternately, laparoscopic sigmoid resection (LSR) compared to open sigmoid resection (OSR) showed that LSR is not superior to OSR for acute symptomatic diverticulitis. Furthermore, laparoscopic lavage was as safe as resection for perforated diverticulitis with peritonitis.[40]
Maneuvers
All colon surgeries involve only three maneuvers that may vary in complexity depending on the region of the bowel and the nature of the disease. The maneuvers are the retraction of the colon, the division of the attachments to the colon, and the dissection of the mesentery.[41] After the resection of the colon, the surgeon normally divides the attachments to the liver and the small intestine. After the mesenteric vessels are dissected, the colon is divided with special surgical staplers that close off the bowel while cutting between the staple lines. After resection of the affected bowel segment, an anvil and spike are used to anastomose the remaining segments of the bowel. Anastomosis is confirmed by filling the cavity with normal saline and checking for any air bubbles.
Bowel resection with colostomy
When excessive inflammation of the colon renders primary bowel resection too risky, bowel resection with colostomy remains an option. Also known as the Hartmann's operation, this is a more complicated surgery typically reserved for life-threatening cases. The bowel resection with colostomy implies a temporary colostomy, which is followed by a second operation to reverse the colostomy. The surgeon makes an opening in the abdominal wall (a colostomy), which helps clear the infection and inflammation. The colon is brought through the opening, and all waste is collected in an external bag.[42]
The colostomy is usually temporary, but it may be permanent, depending on the severity of the case.[43] In most cases, several months later, after the inflammation has healed, the person undergoes another major surgery, during which the surgeon rejoins the colon and rectum and reverses the colostomy.
Prophylactic endoscopic clipping
Prophylactic endoscopic clipping[44] is being researched for diverticulitis.[45]
الشيوع
تصيب التهابات الرتوج عادة من هم في منتصف العمر والأكبر سناً، [46] إلا أنها تصيب من هم أصغر سناً وخاصة ذوي السمنة المتوسطة، وقد يصل أصغر سن للإصابة إلى 20 عاماً.[47]
تنطوي أمراض الرتوج بين سكان البلدان الغربية على القولون السيني (95 ٪ من المرضى). انتشار أمراض الرتوج قد ارتفع من ما يقدر ب 10٪ في عقد 1920 إلى ما يتراوح بين 35 و 50٪ بحلول أواخر عقد 1960. ويعتقد بأن 65٪ من هم أكبر من 85 عاماً لديهم شكل من أشكال أمراض الرتوج في القولون، بينما أقل من 5% ممن أعمارهم أقل من 40 عام تظهر لديهم رتوج في القولون.
أمراض الرتوج في الجانب الأيسر من القولون (غالباً ما تكون على القولون السيني) هو الأكثر شيوعا في الغرب، في حين أن أمراض الرتوج في الجانب الأيمن من القولون هو أكثر انتشارا في آسيا وأفريقيا. 10-25٪ من المرضى الذين يعانون من رتوج القولون سوف يصابون بالتهاب الرتوج في حياتهم.
Diverticulitis most often affects the elderly. In Western countries, diverticular disease most commonly involves the sigmoid colon (95 percent of people with diverticulitis).[48] Diverticulosis affects 5–45% of individuals with the prevalence of diverticulosis increasing with age from under 20% of individuals affected at age 40 up to 60% of individuals affected by age 60.[48]
Left-sided diverticular disease (involving the sigmoid colon) is most common in the West. Right-sided diverticular disease (involving the ascending colon) is more common in Asia and Africa.[49] Among people with diverticulosis, 4–15% may go on to develop diverticulitis.[50]
المصادر
الهامش
- ^ Lee, Kyoung Ho; Lee, Hye Seung; Park, Seong Ho; Bajpai, Vasundhara; Choi, Yoo Shin; Kang, Sung-Bum; Kim, Kil Joong; Kim, Young Hoon (2007). "Appendiceal Diverticulitis". Journal of Computer Assisted Tomography. 31 (5): 763–9. doi:10.1097/RCT.0b013e3180340991. PMID 17895789. S2CID 1027938.
- ^ أ ب Onur MR, Akpinar E, Karaosmanoglu AD, Isayev C, Karcaaltincaba M (February 2017). "Diverticulitis: a comprehensive review with usual and unusual complications". Insights into Imaging. 8 (1): 19–27. doi:10.1007/s13244-016-0532-3. PMC 5265196. PMID 27878550.
- ^ Horton, KM; Corl, FM; Fishman, EK (2000). "CT evaluation of the colon: inflammatory disease". Radiographics. 20 (2): 399–418. doi:10.1148/radiographics.20.2.g00mc15399. PMID 10715339.
- ^ "CT scan of diverticulitis". ClariPACS. 2017. Retrieved 19 June 2017.
- ^ Sai, V. F.; Velayos, F; Neuhaus, J; Westphalen, A. C. (2012). "Colonoscopy after CT Diagnosis of Diverticulitis to Exclude Colon Cancer: A Systematic Literature Review". Radiology. 263 (2): 383–390. doi:10.1148/radiol.12111869. PMC 3329267. PMID 22517956.
- ^ Tursi, A (2015). "The role of colonoscopy in managing diverticular disease of the colon" (PDF). Journal of Gastrointestinal and Liver Diseases. 24 (1): 85–93. doi:10.15403/jgld.2014.1121.tur. PMID 25822438. Archived (PDF) from the original on 2017-08-10.
- ^ Sartelli, Massimo; Weber, Dieter G.; Kluger, Yoram; Ansaloni, Luca; Coccolini, Federico; Abu-Zidan, Fikri; Augustin, Goran; Ben-Ishay, Offir; Biffl, Walter L.; Bouliaris, Konstantinos; Catena, Rodolfo; Ceresoli, Marco; Chiara, Osvaldo; Chiarugi, Massimo; Coimbra, Raul; Cortese, Francesco; Cui, Yunfeng; Damaskos, Dimitris; de Angelis, Gian Luigi; Delibegovic, Samir; Demetrashvili, Zaza; De Simone, Belinda; Di Marzo, Francesco; Di Saverio, Salomone; Duane, Therese M.; Faro, Mario Paulo; Fraga, Gustavo P.; Gkiokas, George; Gomes, Carlos Augusto; Hardcastle, Timothy C.; Hecker, Andreas; Karamarkovic, Aleksandar; Kashuk, Jeffry; Khokha, Vladimir; Kirkpatrick, Andrew W.; Kok, Kenneth Y. Y.; Inaba, Kenji; Isik, Arda; Labricciosa, Francesco M.; Latifi, Rifat; Leppäniemi, Ari; Litvin, Andrey; Mazuski, John E.; Maier, Ronald V.; Marwah, Sanjay; McFarlane, Michael; Moore, Ernest E.; Moore, Frederick A.; Negoi, Ionut; Pagani, Leonardo; Rasa, Kemal; Rubio-Perez, Ines; Sakakushev, Boris; Sato, Norio; Sganga, Gabriele; Siquini, Walter; Tarasconi, Antonio; Tolonen, Matti; Ulrych, Jan; Zachariah, Sannop K.; Catena, Fausto (May 7, 2020). "2020 update of the WSES guidelines for the management of acute colonic diverticulitis in the emergency setting". World Journal of Emergency Surgery. 15 (1): 32. doi:10.1186/s13017-020-00313-4. PMC 7206757. PMID 32381121.
- ^ Peery, Anne F.; Shaukat, Aasma; Strate, Lisa L. (February 28, 2021). "AGA Clinical Practice Update on Medical Management of Colonic Diverticulitis: Expert Review". Gastroenterology. 160 (3): 906–911.e1. doi:10.1053/j.gastro.2020.09.059. PMC 7878331. PMID 33279517.
- ^ أ ب Kruis W, Germer CT, Böhm S, Dumoulin FL, Frieling T, Hampe J, Keller J, Kreis ME, Meining A, Labenz J, Lock JF, Ritz JP, Schreyer A, Leifeld L (November 28, 2022). "German guideline diverticular disease/diverticulitis: Part I: Methods, pathogenesis, epidemiology, clinical characteristics (definitions), natural course, diagnosis and classification". United European Gastroenterology Journal. 10 (9): 923–939. doi:10.1002/ueg2.12309. PMC 9731664. PMID 36411504.
- ^ Kruse, E; Leifeld, L (April 2015). "Prevention and Conservative Therapy of Diverticular Disease". Viszeralmedizin. 31 (2): 103–6. doi:10.1159/000377651. PMC 4789966. PMID 26989379.
- ^ Klarenbeek, B. R.; De Korte, N; Van Der Peet, D. L.; Cuesta, M. A. (2011). "Review of current classifications for diverticular disease and a translation into clinical practice". International Journal of Colorectal Disease. 27 (2): 207–214. doi:10.1007/s00384-011-1314-5. PMC 3267934. PMID 21928041.
- ^ خطأ استشهاد: وسم
<ref>غير صحيح؛ لا نص تم توفيره للمراجع المسماةauto - ^ خطأ استشهاد: وسم
<ref>غير صحيح؛ لا نص تم توفيره للمراجع المسماةauto1 - ^ "CKS is only available in the UK".
- ^ Strate LL, Morris AM (April 2019). "Epidemiology, Pathophysiology, and Treatment of Diverticulitis". Gastroenterology. 156 (5): 1282–1298.e1. doi:10.1053/j.gastro.2018.12.033. PMC 6716971. PMID 30660732.
- ^ Rottier, SJ; van Dijk, ST; van Geloven, AAW; et al. (July 2019). "Meta-analysis of the role of colonoscopy after an episode of left-sided acute diverticulitis". The British Journal of Surgery. 106 (8): 988–997. doi:10.1002/bjs.11191. PMC 6618242. PMID 31260589.
- ^ أ ب ت ث ج "Diverticulitis prognosis".
- ^ أ ب Linzay, Catherine D.; Pandit, Sudha (January 14, 2023). "Acute Diverticulitis". StatPearls. StatPearls Publishing. PMID 29083630.
- ^ Hanna, Mark H; Kaiser, Andreas M (March 7, 2021). "Update on the management of sigmoid diverticulitis". World Journal of Gastroenterology. 27 (9): 760–781. doi:10.3748/wjg.v27.i9.760. PMC 7941864. PMID 33727769.
- ^ Rook, Jordan M.; Dworsky, Jill Q.; Curran, Thomas; Banerjee, Sudeep; Kwaan, Mary R. (May 1, 2021). "Elective surgical management of diverticulitis". Current Problems in Surgery. 58 (5) 100876. doi:10.1016/j.cpsurg.2020.100876. PMID 33933211.
- ^ Sartelli, Massimo; Weber, Dieter G.; Kluger, Yoram; et al. (May 7, 2020). "2020 update of the WSES guidelines for the management of acute colonic diverticulitis in the emergency setting". World Journal of Emergency Surgery. 15 (1): 32. doi:10.1186/s13017-020-00313-4. PMC 7206757. PMID 32381121.
- ^ أ ب Kruse, Elena; Leifeld, Ludger (April 28, 2015). "Prevention and Conservative Therapy of Diverticular Disease". Viszeralmedizin. 31 (2): 103–106. doi:10.1159/000377651. PMC 4789966. PMID 26989379.
- ^ أ ب van Dijk, S. T.; Rottier, S. J.; van Geloven, A. A. W.; Boermeester, M. A. (February 28, 2017). "Conservative Treatment of Acute Colonic Diverticulitis". Current Infectious Disease Reports. 19 (11): 44. doi:10.1007/s11908-017-0600-y. PMC 5610668. PMID 28942590.
- ^ Spirt, Mitchell (2010). "Complicated Intra-abdominal Infections: A Focus on Appendicitis and Diverticulitis". Postgraduate Medicine. 122 (1): 39–51. doi:10.3810/pgm.2010.01.2098. PMID 20107288. S2CID 46716128.
- ^ "Diverticulitis – Diagnosis and treatment – Mayo Clinic". www.mayoclinic.org.
- ^ أ ب ت Sartelli, Massimo; Weber, Dieter G.; Kluger, Yoram; et al. (2020-05-07). "2020 update of the WSES guidelines for the management of acute colonic diverticulitis in the emergency setting". World Journal of Emergency Surgery. 15 (1): 32. doi:10.1186/s13017-020-00313-4. ISSN 1749-7922. PMC 7206757. PMID 32381121.
- ^ Peery, Anne F.; Shaukat, Aasma; Strate, Lisa L. (February 12, 2021). "AGA Clinical Practice Update on Medical Management of Colonic Diverticulitis: Expert Review". Gastroenterology. 160 (3): 906–911.e1. doi:10.1053/j.gastro.2020.09.059. PMC 7878331. PMID 33279517.
- ^ أ ب Nascimbeni, R.; Amato, A.; Cirocchi, R.; et al. (2021). "Management of perforated diverticulitis with generalized peritonitis. A multidisciplinary review and position paper". Techniques in Coloproctology. 25 (2): 153–165. doi:10.1007/s10151-020-02346-y. ISSN 1123-6337. PMC 7884367. PMID 33155148.
- ^ Bianchi, M.; Festa, V.; Moretti, A.; Ciaco, A.; Mangone, M.; Tornatore, V.; Dezi, A.; Luchetti, R.; De Pascalis, B.; Papi, C.; Koch, M. (April 28, 2011). "Meta-analysis: long-term therapy with rifaximin in the management of uncomplicated diverticular disease". Alimentary Pharmacology & Therapeutics. 33 (8): 902–910. doi:10.1111/j.1365-2036.2011.04606.x. PMID 21366632.
- ^ "Mesalazine: A medicine that treats inflammatory bowel conditions including ulcerative colitis and Crohn's disease". 21 July 2021.
- ^ Lenza, Christopher; Das, Kiron M. (2011). "Mesalamine in the Treatment of Diverticular Disease". Journal of Clinical Gastroenterology. 45: S53–S61. doi:10.1097/MCG.0b013e3182107a37. S2CID 78890788.
- ^ Iannone, Andrea; Ruospo, Marinella; Wong, Germaine; Barone, Michele; Principi, Mariabeatrice; Di Leo, Alfredo; Strippoli, Giovanni F. M. (September 16, 2018). "Mesalazine for People with Diverticular Disease: A Systematic Review of Randomized Controlled Trials". Canadian Journal of Gastroenterology & Hepatology. 2018 5437135. doi:10.1155/2018/5437135. PMC 6167594. PMID 30320044.
- ^ Peery, Anne F. (November 12, 2022). "New German guidelines for the management of diverticulitis". United European Gastroenterology Journal. 10 (9): 913–914. doi:10.1002/ueg2.12331. PMC 9731652. PMID 36302089.
- ^ أ ب خطأ استشهاد: وسم
<ref>غير صحيح؛ لا نص تم توفيره للمراجع المسماةJAMA2014 - ^ What's the diverticulitis surgery? Archived 2010-02-27 at the Wayback Machine Digestive Disorders portal. Retrieved on 2010-02-23
- ^ Merck, Sharpe & Dohme. "Diverticulitis treatments" Archived 2010-03-06 at the Wayback Machine 2010-02-23.
- ^ Diverticulitis: Treatment & Medication Archived 2010-03-16 at the Wayback Machine eMedicine. 2010-02-23
- ^ Diverticulitis Surgery Archived 2010-02-12 at the Wayback Machine 2010-02-23
- ^ Gupta, Aditya K.; Chaudhry, Maria; Elewski, Boni (2003). "Tinea corporis, tinea cruris, tinea nigra, and piedra". Dermatologic Clinics. 21 (3): 395–400, v. doi:10.1016/S0733-8635(03)00031-7. PMID 12956194.
- ^ Ahmed, Ali Mahmoud; Mohammed, Abdelrahman Tarek; Mattar, Omar Mohamed; et al. (1 July 2018). "Surgical treatment of diverticulitis and its complications: A systematic review and meta-analysis of randomized control trials". The Surgeon. 20 (6): 372–383. doi:10.1016/j.surge.2018.03.011. PMID 30033140. S2CID 51709390.
- ^ Bowel resection procedure Archived 2010-01-29 at the Wayback Machine Encyclopedia of surgery. Retrieved on 2010-02-23
- ^ Diverticulitis treatments and drugs Archived 2010-02-12 at the Wayback Machine Mayo Clinic. 2010-02-23
- ^ Vermeulen J, Coene PP, Van Hout NM, van der Harst E, Gosselink MP, Mannaerts GH, Weidema WF, Lange JF (July 2009). "Restoration of bowel continuity after surgery for acute perforated diverticulitis: should Hartmann's procedure be considered a one-stage procedure?". Colorectal Disease. 11 (6): 619–24. doi:10.1111/j.1463-1318.2008.01667.x. PMID 18727727. S2CID 20693528.
- ^ Xavier AT, Campos JF, Robinson L, Lima EJ, Da Rocha LC, Arantes VN (November–December 2020) [30 July 2020 (online publication)]. "Endoscopic clipping for gastrointestinal bleeding: emergency and prophylactic indications". Annals of Gastroenterology. 33 (6): 563–570. doi:10.20524/aog.2020.0526. PMC 7599350. PMID 33162733.
- ^ "Prophylactic Endoscopic Clipping of Colonic Diverticula (PECoD) V8". Health Research Authority.
- ^ Cole CD, Wolfson AB (2007). "Case Series: Diverticulitis in the Young". J Emerg Med. 33: 363. doi:10.1016/j.jemermed.2007.02.022. PMID 17976749.
- ^ "Disease Of Older Adults Now Seen In Young, Obese Adults". Retrieved 2007-11-19.
- ^ أ ب Nallapeta, Naren S.; Farooq, Umer; Patel, Krunal (2022), Diverticulosis, Treasure Island (FL): StatPearls Publishing, PMID 28613522, https://www.ncbi.nlm.nih.gov/books/NBK430771/, retrieved on 2022-10-18
- ^ خطأ استشهاد: وسم
<ref>غير صحيح؛ لا نص تم توفيره للمراجع المسماةFel2010 - ^ Pemberton, John H (16 June 2016). "Colonic diverticulosis and diverticular disease: Epidemiology, risk factors, and pathogenesis". UpToDate. Archived from the original on 2017-03-14. Retrieved 13 March 2017.